Article by Dr Hugh Porter (Northern Beaches Obstetrician)

Recent social media trends have highlighted the importance of a woman’s ‘birthing experience’. In this blog Dr Hugh Porter discusses pain relief options in labour, vaginal birth after caesarean section (VBAC), and the relatively new trend of ‘maternal assisted’ caesarean sections.
Pain relief options in labour
Every woman’s experience of labour is different. Some women aim to labour naturally without any pain relief, and others elect for an epidural as soon as they arrive in the hospital. As a private obstetrician, I am happy to support my patients’ choices when it comes to pain relief. There are loads of pain relief options in labour, and I like to educate my patients on all of them:
- Natural methods (water immersion, calm and soothing music, breathing techniques etc)
- The mind is a powerful thing! Discussing your birth plan and preparing yourself mentally for labour before the big day is crucial for success.
- There are many pre-labour courses on the Northern Beaches that cover natural pain relief techniques. Some of my favourites are:
- TENS machine
- Electrical nerve stimulation via sticky pads placed on the lower back. Thought to work by blocking pain signals from making it to the brain. In my experience, tens machines work very well in the early stages of labour (ideally started at home, before you even make it to hospital)
- Sterile water injections
- A medical procedure in which small amounts of sterile water are injected into your lower back or abdomen during labour. The injections are given using a fine needle and syringe, and the water is injected just under
the skin.
- They feel like a bee-sting (I know, I’ve tried them!), and after the initial shock, can decrease contraction pain in some women.
- A medical procedure in which small amounts of sterile water are injected into your lower back or abdomen during labour. The injections are given using a fine needle and syringe, and the water is injected just under
- Nitrous oxide gas
- The same gas used at the dentist, also known as ‘laughing gas’. Safe for mum and bub, nitrous oxide is breathed in via a mouthpiece during each contraction. It’s short acting, so the euphoric feeling wears off when you stop breathing on the gas. It doesn’t work for everyone, but for some women, nitorus oxide is enough to take the edge off the contractions.
- Medications (Panadol, endone/morphine)
- Highly effective in preventing or removing pain. Endone or morphine are very effectively in early labour, but are typically avoided in the few hours before baby is born to avoid making baby drowsy.
- Epidural
- Administered by your friendly anaesthetist, a well-functioning epidural blocks all pain signals below your belly button. You’re less mobile with an epidural in, but will feel significantly more comfortable. Most epidurals allow mum to press a button and top up her pain relief as required.
Vaginal Birth after Caesarean Section (VBAC)
- What is it?
- VBAC stands for Vaginal Birth After Caesarean, which refers to the delivery of a baby vaginally by a woman who has previously had a caesarean. In the past, it was believed that once a woman had a caesar, all future deliveries would also require a caesar. With advancements in medical technology and improved understanding of the risks and benefits, many women who have had a caesarean section may be candidates for a VBAC.
- Will my VBAC attempt be successful?
- On average, about 60-70% of women who attempt a VBAC are successful meaning they deliver vaginally without requiring a repeat caesarean. However, the success rate may be lower or higher depending the following (individual) factors:
- Reason for the previous caesarean: Your VBAC is more likely to work if your cervix dilated in the previous pregnancy, and the reason for your caesar was for ‘foetal distress’, rather than cephalopelvic disproportion (or ‘stalled labour’).
- Previous vaginal birth: If you have had a previous vaginal birth, your chance of a successful VBAC is significantly higher.
- Maternal age: Older women may have a lower success rate for VBAC than younger women.
- Induction of labour: The use of medications to induce labour (eg syntocinon) may increase the risk and decrease the success rate of VBAC.
- Size of the baby: Women carrying larger babies may have a lower success rate for VBAC.
- Weight. Obesity can decrease your chance of a successful VBAC.
- On average, about 60-70% of women who attempt a VBAC are successful meaning they deliver vaginally without requiring a repeat caesarean. However, the success rate may be lower or higher depending the following (individual) factors:
- Is a VBAC safe?
- The reason some obstetricians do not offer VBAC is that there are potentially very serious risks associated. The most severe complication of an attempted VBAC is a uterine rupture. This risk however, if labour is approached in safe way, is very low (1:200 if you labour on your own, and 1:100 if you are induced).
- Who is it suitable for?
- Candidates for VBAC should have:
- Their uterus closed in two layers (standard practice, and we can check the operation report from your previous caesar).
- An 18-month interval between your last baby being born, and this baby being born. This gives your uterine scar time to heal.
- Delivery in a hospital with access to emergency operating theatres
- continuous monitoring of the baby’s heart rate in labour – via a “CTG”.
- No other medical reason why you can’t have a vaginal birth (eg low lying placenta, growth restricted baby etc).
- A lengthy discussion with your obstetrician regarding the risks and benefits of trying for a VBAC.
- Candidates for VBAC should have:
Maternal assisted Caesarean section (MACS)
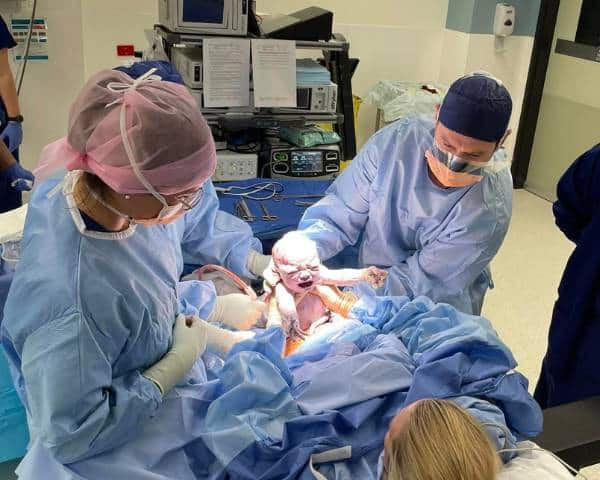
- What is it?
- At a maternal assisted caesarean section, the mother literally scrubs with her surgeon. The surgeon will perform the majority of the procedure, however at the time of the delivery, mum is empowered to reach over the drapes, and deliver her own baby onto her chest.
- What are the benefits?
- MACS have been shown to promote a feeling of control. The can be a very empowering experience for some women, and may help to promote bonding between the mother and baby.
- Who is it for?
- MACS are particularly good for women who desperately wanted a vaginal delivery, but are required to have a caesarean for a medical reason (for example a low lying placenta).
- Mothers who had a traumatic first birth, or feel like they lost control also find this procedure particularly beneficial.
- While MACs can be a positive experience for some women, they are not appropriate for all women or all situations. MACs may not be recommended if the mother has a medical condition that would make it difficult for her to participate in the delivery, or if the baby is in distress and requires a quick delivery.
- What are the risks
- The most serious risk associated with maternal assisted caesarean section is infection. At Northern Beaches Hospital, a specific safety protocol has been carefully developed to minimise this risk.

Dr Porter sees both private and public patients and has consulting rooms inside Northern Beaches Hospital.
If you are interested in more information about pain relief options in labour, vaginal birth after caesarean section (VBAC), or a maternal assisted caesarean section, please contact:
Dr Hugh Porter – Sydney Babies
www.sydneybabies.com.au
Check out his Instagram: https://www.instagram.com/drhughporter/
Mums of the Northern Beaches are invited to join local father and obstetrician Dr Hugh Porter from Northern Beaches Hospital via Facebook Live on Wednesday 28th June at 8pm. Event details here.



